
________________________________________________________________
Notes to accompany lecture to 2nd year City University undergraduates
Dr Simon Barnard Phd BSc FCOptom FAAO DCLP
Index
Table of Contents
Introduction
The nerve
Blood supply
General clinical features of disorders of the optic nerve.
Classification of diseases affecting the optic nerve
Developmental anomalies
Aplasia & hypoplasia.
Colobomas
Morning glory syndrome
Optic nerve pit
Myelinated nerve fibres
Retarded myelination
Glial remnants
Congenital swelling of the optic disc (pseudo - papilloedema)
Congenital and myopic crescents (conus)
Tilted disc
Vascular anomalies
Aneurysms & subarachnoid haemorrhage
Ischaemia & infarction of the nerve tissue
Sclerosis of the major arteries
Glaucoma
Demyelinating and inflammatory diseases
Toxic including iatrogenic and nutritional disorders
Tumours & cysts
Drusen of the Optic Disc
Trauma
Optic Atrophy
"Choked disc"
Further reading
The nerve
The O.N. is a tract consisting mainly of the axons of the ganglion cells of the retina . These axons converge on the optic disc, which is approximately 1.5mm in diameter, pierce the sclera at the lamina cribosa, a sieve-like structure, then form bundles of myelinated nerve fibres separated by connective tissue septa. Largely because of the presence of the myelin sheaths and the connective tissue septa behind the level of the lamina cribosa, the optic nerve has a greater diameter at the point at which it leaves the globe than at it's head (the optic disc).
Each optic nerve is encased in sheaths continuous with and similar to the meninges of the cranium (pia, arachnoid, and the dura).
The optic nerve may be considered as consisting of four parts:-
(1) the head & ocular portion which traverses the sclera
(2) the orbital portion, which is about 3cm in length and has an S-shaped course so that the globe is able to move freely
(3) the portion in the optic canal, which is some 5-7mms long
(4) an intracranial portion which extends from the optic canal to the anterior part of the optic chiasm
The arterial supply to the optic nerve anterior to the lamina cribosa is derived from the short ciliary arteries. Immediately behind the lamina cribosa vessels derived from the Circle of Zinn, which is itself supplied by the short ciliary arteries, enter the optic nerve. The orbital portion of the optic nerve derives its blood supply from the pial circulation and perhaps also to some extent from the ophthalmic artery and its branches, including the central retinal artery. That portion of the optic nerve lying in the optic canal derives its arterial blood supply from the ophthalmic artery, whilst the intra-cranial part of the optic nerve is supplied centripetally through the pial vessels. Venous drainage from the ocular and orbital portions of the optic nerve is chiefly into the central retinal vein.
General clinical features of disorders of the optic nerve.
Unilateral visual failure unassociated with ophthalmoscopic signs may be due to optic nerve disease. However when the cause is due to toxic or systemic disease, the visual loss may be bilateral.
Consider visual acuities, contrast sensitivity, colour vision, visual fields and pupil reactions. If visual failure is complete the direct pupil response to light will be lost and the pupil may be dilated. If visual loss is less severe, the pupil may show loss of sustained direct response to light stimulus and a rhythmical contraction of abnormal amplitude (hippus).
Classification of diseases affecting the optic nerve
May be based on aetiologic factors and/or clinical appearance:-
Developmental anomalies
Vascular disorders
Glaucoma
Demyelinating and inflammatory disease
Toxic including iatrogenic disorders
Tumours & cysts
Drusen
Trauma
Aplasia (rare) and hypoplasia is a failure of the optic nerve to develop. Hypoplasia is bilateral in about 60% of cases. May be a sporadic developmental anomaly or hereditary . Small grey disc often surrounded by yellow halo of hypopigmentation due to choroidal and RPE abnormality , reduced V.A. and a variety of visual field defects.
Incomplete closure of foetal cleft thus appearing inferiorly. May be associated with choroidal/iris coloboma. Field defect corresponds to the area of projection of the missing fibres. Visual acuity may be affected.

Rare dysplastic coloboma of optic disc. ON head enlarged and cupped with hyaloid remnants within its base. Usually unilateral. Vision grossly impaired.
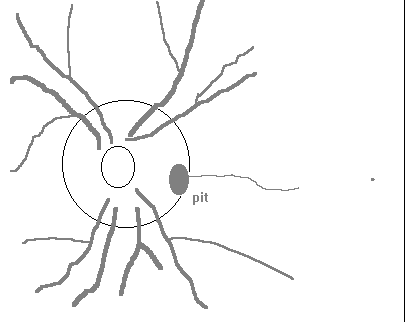
Not related to coloboma. Rare (1 per 11,000) . Bilateral in 15% of cases. Occasionally more than one hole. Usually positioned inferotemporal quadrant of papilla. Size varies from 0.1 to 0.7 disc diameter (average 0.3). Depth varies from 0.5D to 20D. Usually grey in colour. Visual field defects of various types. Cause not certain. Possible sequel is serous retinal detachment.
Myelination of the optic nerve develops embryologically from a posterior to anterior direction. The fibres are grossly Myelinated in the intracranial and intracanal portions of the optic nerve by the seventh month but myelin does not usually reach the lamina cribosa until full term. I some instances the myelin does not stop short at the lamina cribosa but continues into the eye, appearing on ophthalmoscopic examination as bright white flame-shaped streaks, usually contiguous with the margin of the optic disc. These streaks follow the normal course of the retinal nerve fibres and are situated superficially on the disc and retina and hence may cover some of the retinal blood vessels. They give rise to field defects corresponding to their area of projection into the visual field.
A number of observers have reported the appearance of the optic disc as being grey in premature and some full- term infants.
Possible cause of strabismus ?
The posterior portion of the hyaloid artery may persist extending into the vitreous from the disc surrounded by glial tissue (Bergmeister's papilla). Sometimes sheets of persistent glial tissue are seen covering the optic disc in part or as a whole and producing a slightly grey filmy (gossamer) appearance.
Congenital swelling of the optic disc (pseudo - papilloedema)
This is a physiological variation from the norm seen fairly frequently in patients with high axial hypermetropia.
Margins of disc appear blurred and disc tissue somewhat elevated. Major points in favour of diagnosis of pseudo-papilloedema as opposed to pathological "choked-disc" are (1) the type of eye (hypermetropic ?) (2) absence of exudates or haemorrhages (3) a normal visual field with a small-sized physiological blind spot (3) normal fluorescein angiogram
Congenital and myopic crescents (conus)
The ophthalmoscopic appearance of the margin of the optic disc is determined to a large extent by the distances from the disc margin at which the RPE, Bruch's membrane and the choroid terminate. In axial myopes these tissues are often absent over a crescent-shaped area on the temporal side of the disc (myopic crescent). This is probably due to chorioretinal atrophy and/or traction of the retina and choroid on the nasal side due to elongation of the globe at the posterior pole.
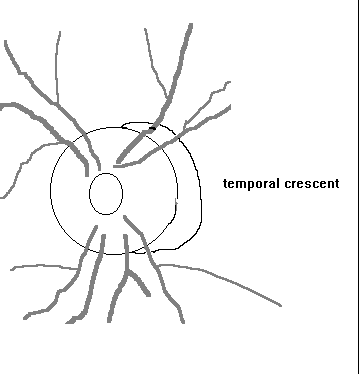
Occasionally the optic nerve leaves the sclera more obliquely than usual giving rise to an inferior or superior conus. Visual field anomalies may be present.
Aneurysms & subarachnoid haemorrhage
Aneurysms involving ON may arise from internal carotid, anterior cerebral, anterior communicating, and occasionally from ophthalmic artery. Because aneurysms exert their effect by slow growth they may give rise to the same symptoms as tumours i.e. compression Þ visual field defects and primary optic atrophy. When they bleed they give rise to the same symptoms as sub-arachnoid haemorrhages. Symptoms suggestive of an aneurysm are those of sudden onset which vary from day to day. Apart from an aneurysm, subarachnoid haemorrhage may result from trauma, tumours, the breakthrough of a intracerebral haemorrhage, or spontaneously. Always check that the limiting edge of a subconjunctival haemorrhage is visible.
Ischaemia & infarction of the nerve tissue
Occlusive disease (either inflammatory or degenerative in origin) of the arteries supplying the optic nerve is a frequent cause of damage. Aetiologies include giant cell arteritis, CRA occlusion by embolism or thrombus, thrombosis of CRV, and occlusion of ophthalmic artery or internal carotid, most commonly by atheromatous plaque formation. Temporal arteritis may be accompanied by giant cell arteritis of posterior ciliary arteries resulting in ischaemic optic neuropathy. Giant cell arteritis usually affects patients
over 50 years of age. Where it includes temporal arteritis the symptoms may include unilateral headache and tenderness of the temple. At first there may be dimming of the vision followed by complete amaurosis. Other inflammatory diseases affecting the arteries supplying the optic nerve include polyarteritis nodosa, thromboangiitis obliterans, optic disc vasculitis and syphilitic meningitis. Ischaemic optic neuropathy is not always the result of giant cell arteritis (e.g. it may be caused by arteriosclerotic occlusive disorders of the posterior ciliary arteries.
Sclerosis of the major arteries
Some sclerosed vessels (e.g. internal carotid and anterior cerebral arteries) can cause visual impairment by direct pressure on the optic nerve. This may give rise to episodic loss of vision but rarely leads to complete amaurosis.
(see other lectures)
Demyelinating and inflammatory diseases
(see other lectures)
Toxic including iatrogenic and nutritional disorders
Many substances can affect the function of the optic nerve and may give rise visual field defects and colour vision anomalies.
Examples include: Tobacco, ethyl and methyl alcohol; sedative drugs such as morphia and phenyprazine, anti-infective drugs such as chloramphenicol, and other drugs such as digoxin, thyroxin, nicotinic acid, quinine derivatives and salicylic acid;
metals such as lead, thallium and arsenic.
Optic neuritis of nutritional origin include beri-beri and pernicious anaemia.
Intrinsic - e.g. gliomas and meningiomas originating from nerve tissue
Extrinsic e.g. meningiomas of sphenoidal ridge or olfactory groove, pituitary adenomas and some metastatic tumours. Tumours in the orbit may interfere with ocular motility and cause proptosis and additionally interfere with vision if they affect the ON conductive system
This degenerative condition consists of a build up of spheres of hyaline material in front of the lamina cribosa. As they enlarge they give rise to an elevation of the optic disc and a blurring of the margins. When they are situated superficially the ophthalmoscopic appearance is of white or white-yellow spheres which have a sheen or appear translucent if illuminated from one side. If they are deep they may not be observable with the ophthalmoscope and cause a misdiagnosis of papilloedema.
Can be progressive. Visual field defects. Usually bilateral.
A small percentage of head injuries can produce damage to the optic nerve which do not have the Schwann sheaths necessary for effective regeneration of the nerves.
Observed clinically as pallor of the disc
PRIMARY - disc margins are distinct
SECONDARY - disc margins indistinct - such cases result from previous oedema or inflammation of the nerve head
CONSECUTIVE (or ascending) optic atrophy is that which occurs secondary to retinal disease in which ganglion cells have been destroyed e.g. CRA occlusion
DESCENDING optic atrophy may result from lesions affecting the orbital, optic canal portion, or intracranial portion of ON
May be due to papilloedema or papillitis. Ophthalmoscopic appearance indistinguishable .
Papilloedema is a non-inflammatory swelling of optic nerve head with abnormal elevation of disc and blurring of margins. As condition progresses haemorrhages (usually flame shaped) may appear on the nerve head and surrounds. The oedema may spread into the surrounding retina causing concentric folds. There is a loss of spontaneous venous pulsation. Commonest causes include Grade 4 vascular hypertension and raised intracranial pressure.
In all but the late stages central vision and colour vision unaffected. Enlarged blind spot.
Papillitis is an active inflammation of nerve head (an optic neuritis). Central vision affected including field loss, colour vision disturbances, and reduced vision. Pain on movement of eye. Possible causes include MS.
Alexander L. (1995) Primary Care of the Posterior Segment. Appleton & Lang, Norwalk
Barnard N.A.S. (1989) Congenital pit of the optic nerve. Ophthal.Physiol. Opt, 9, 324-326
Kanski J. (1992) , Clinical Ophthalmology. Chapter on Neuro-ophthalmology, Butterworth- Heinemann, Oxford
Further questions ?… contact e-mail sb@eye-spy.co.uk